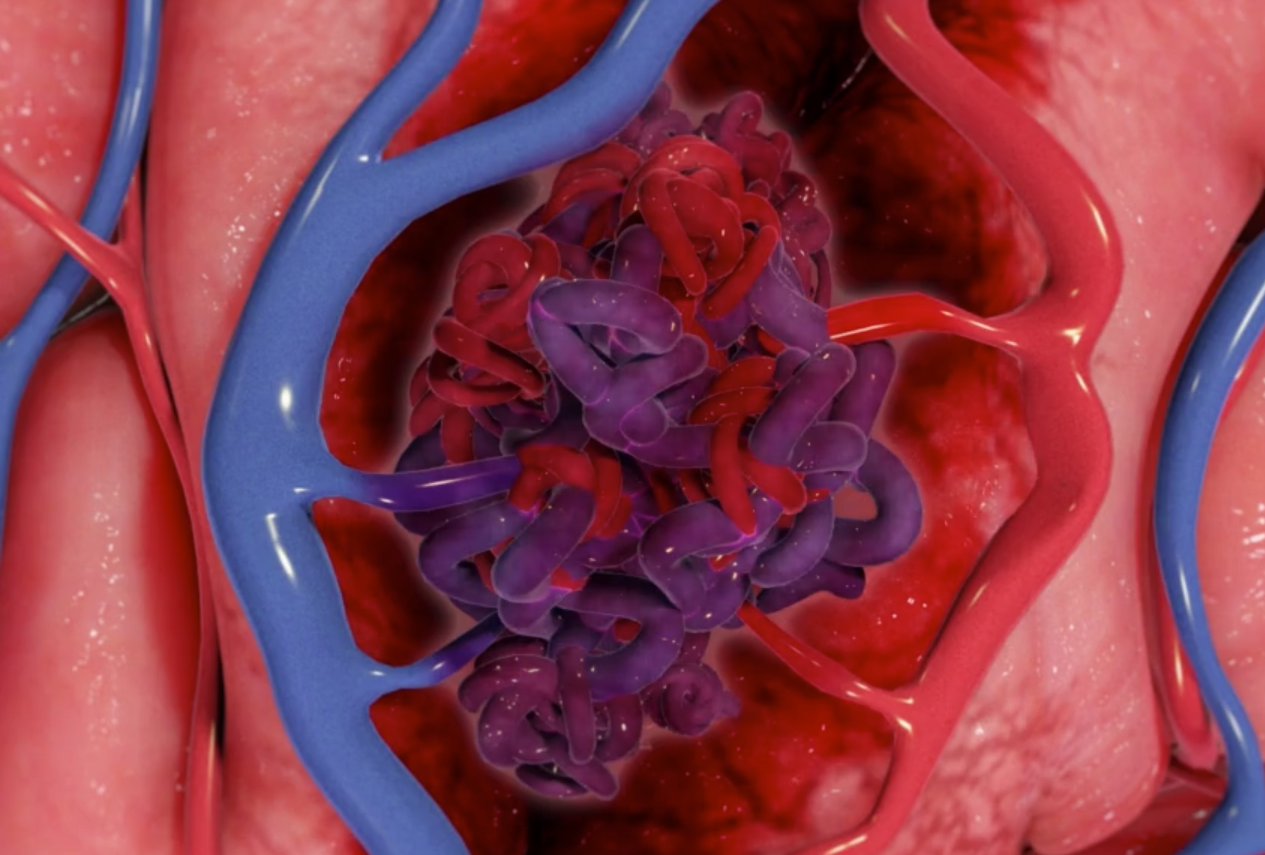
Arteriovenous Malformation Treatment
When deciding on whether to treat an un-ruptured AVM, it is necessary to consider the estimated lifetime risk of rupture compared to the estimated risk of treatment.
The size, location, and venous drainage of an AVM are taken into account when determining the risk from surgical removal.
With some AVMs the estimated risk of surgical removal is significantly smaller than the lifetime risk of rupture and therefore surgical removal is a recommended option. Whereas other AVMs are too risky to resect surgically and it may be safer not to operate on them.
Micro-surgery is still considered the best treatment option when it’s performed safely. This is because it carries around 95% chance of instant cure. In some cases, microsurgery is too risky and other treatment options can be considered. These include stereotactic radiosurgery (SRS) or embolisation.
Stereotactic radiosurgery
Stereotactic radiosurgery involves using computer guidance to concentrate beams of radiation to the AVM. This slowly causes abnormal vessels to close off. The success rate from SRS is generally lower than microsurgery. It can also take up to 3 years before the AVM is cured and during this period the AVM can still rupture.
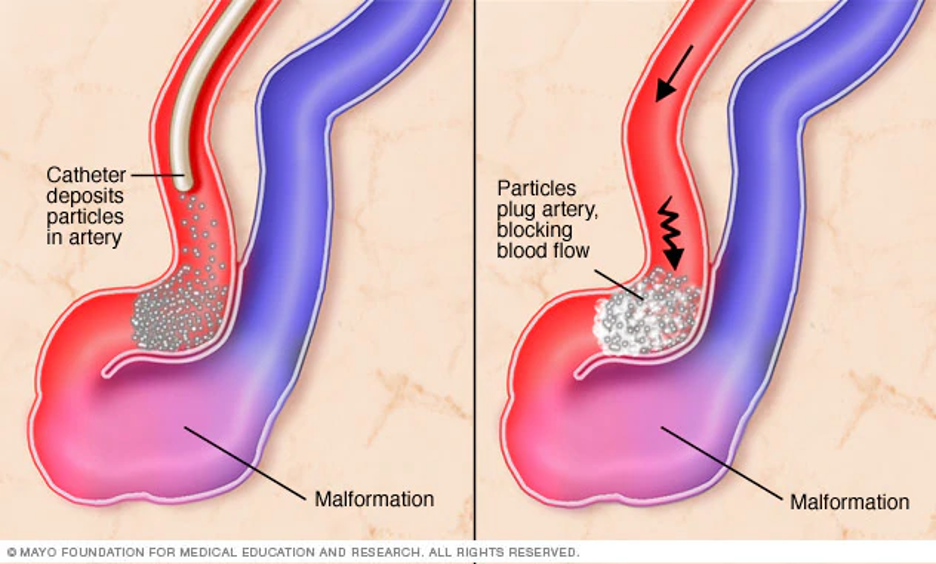
Embolisation
Embolisation involves injecting liquid glue or particles into the AVM. This method inserts microcatheters through an artery in the groin. The success rate of embolisation alone in curing an AVM is often poor. Embolisation can still be used in combination with microsurgery or SRS.
The decision to treat an un-ruptured AVM must be taken by the patient. This follows extensive discussions and guidance from an experienced multi-disciplinary team consisting of a cerebrovascular neurosurgeon, an interventional neuroradiologist and a radiation therapist.
Click here to return to the cerebrovascular diseases page.